Research Article
Present Situation of Cutaneous Leishmaniasis in Balochistan, Pakistan
Sandflies, Leishmaniasis and Mosquitoes Lab./Zoology, University of Balochistan, Quetta, Pakistan
Leishmaniasis is a protozoal disease. It is initiated when the extracellular, flagellated promastogote form of Leishmania is injected into human skin during a sandfly bite. Macrophages or other phagocyte cells, within which the parasites transform into the intracellular amastigote form, rapidly engulf the organisms. Leishmania needs a mammalian species, a reservoir, to maintain its parasitic population. Small terrestrial rodents have been reported infected. Some present cutaneous lesions on the tail but in some specimens, the infection remain a symptomatic.
The status of leishmaniasis in Balochistan has been changing with years. Cutaneous leishmaniasis (CL) is endemic in the Province. Nagi and Nasimullah[1] reported the cases of visceral leishmaniasis (VL) in Balochistan. Most of the cases of VL have been reported from the northern areas of the country[2-14], from Multan[15], Karachi[16, 17] and from eastern and northern parts of the country by Rab[9]. Cutaneous leishmaniasis was reported from Multan by Malik et al.[18] and from Karachi by Nawab et al.[19]. Reviews on leishmaniasis in Pakistan have been published by Haq[20], Munir et al.[21], Masoom and Marri[22], W.H.O.[23] and Yasinzai et al.[24]. In few and old known foci of the Province, the epidemiology of CL have been studied since the early 1980`s. Informative reports were published by AslamKhan and Rafiq[25], Jan[26], Burney and Lari[27], Rab et al.[28, 29], Ahmed[30], Ghazi and Ali[31] Jan et al.[32]. These surveys were carried out in limited areas and for during short period. With the continuous incoming of refugees from Afghanistan especially Pashtoon, Uzbek, Tajek, Turkmen and Persian and from Iran Hazara tribe in to Balochistan Province, the incidence of the disease in the Province has flared up. In view of the reports of the new cases of CL in various areas of the Province and the insufficient reports of the said workers (loc. cit.), led the author to undertake the study of the prevalence of CL, rodents and sandflies in the whole of the Province. It was aimed in the study to determine the age and sex of the CL patients, clinical characteristics, new endemic foci and the prevalence of the species of the rodents and sandflies of the Province which was poorly documented until then. Results of the present study are communicated in the present paper.
The author conducted field surveys during 1996-2001 in the whole of the Balochistan Province. The region has a desert climate, very hot in summer and quite cold in winter. In 1996-2001, the maximum and minimum mean monthly temperatures were 43.8°C and 9.3°C in May to August and December to February, respectively. The total annual rainfall was 88 mm. Minimum mean monthly relative humidity was 28% (May to August) and the maximum was 76% (December to February). In the study area the agricultural population is minimum and most of the houses are made up of mud. Livestock include dogs, donkeys, cattle and cats. Each town /locality was twice visited every year of active season of sandflies. The distribution of recorded CL cases during the study period in various Government Hospitals and Private Clinics of the Province were taken into account. Visits to schools were also conducted. In addition, a brief lecture was delivered in each class about the shape, size and habitat, biting habits of Phlebotomine sandflies and its vectoral role in the spread of the disease. A photograph of sand fly was also shown to the students. Clinical symptoms of the disease and role of domestic dogs and other mammals especially rodents were also explained. In order to control the sand flies and the disease, use of mosquito nets, regular spraying of insecticides in store, washrooms and bedrooms were advised. Emphasis was also made for individual clothing prophylaxis, use of lemon oil[33, 34] and use of citrus leaves on the open parts of the body[35]. Intramuscular meglumine antimonate (Glucantime) injection was recommended for the treatment of CL. Government servants and laborers of other Provinces with CL infection working in the endemic areas of the Province were also taken into account. A questionnaire of each CL patient was filled in having data regarding sex, age, duration and number of lesion, clinical aspects, therapeutic regimen, length of residence in the area, migratory history and presence of dogs and other domestic animals in the surrounding area. Infected subjects were taken to the nearby Government hospital /dispensary for taking biopsy of the edge of active lesion. The procedure and techniques described by WHO[36] were followed. Smears were prepared from scrapping of the edge of the lesion, fixed in methanol, stained with Giemsa and examined under a light microscope for the presence of amastigotes. Sandflies were collected through aspirator and sticky and light traps from indoors and outdoors. Rodents were trapped in locally made traps with spring-operated doors. They were placed amidst active colonies of rodent burrows. Pieces of cheese, carrot and bread smeared with butter were used as bait. The animals caught were examined for sores and scars. Species identification of sandflies[37-40] and rodents were done after following keys. Giemsa preparations from active lesions of human patients and rodents were examined under microscope for amastigotes. The techniques discussed by Rab et al.[28] were generally followed.
Most of the infected persons were found in the new endemic foci viz., Adampur, Awaran, Bhag, Belpat, Chilgiri, Dashte Kuddan, Dhadar, District of Dera Murad Jamali, Hairdin, Jafarabad, Jangal Pir Alizai, JhalJhao, Kahan, Khuzdar, Lehri, Mand, Maiwand, Mashkey, Naillaint, Nanasaheb ziarat, Ornach, Panjgour, Parom, Pishin, Rakhni, Sohbatpur, Tump, Turbat, Usta Mohammad, Winder and Wadh localities.
| Table 1: | Incidence of Cutaneous leishmaniasis in Balochistan Province, age wise |
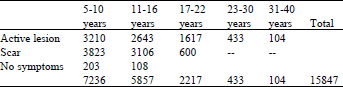 | |
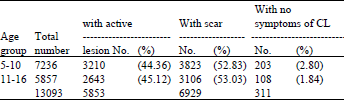
High infection rate of CL was also observed in old foci viz., Bela, Chaman, Dera Bugti, Duki, Kohlu, Las Bella, Quetta and Sibi localities. A total number of 15847 human subjects were recorded, 8007(50.5%) were found with active lesions, seven thousand five hundred twenty nine (47.5%) were observed with scars resulting from leishmania ulcer and 311(1.96%) with no symptoms (Table 1 and 2). Schools surveys (Table 3) revealed that 5853 children out of 13093 school children examined had active lesions (44.70%), 6929 (52.92%) had scars resulting from CL ulcer, three hundred eleven were found with no symptoms of CL. 3210 (20.25 %) children with active lesions were found from the age group of 5-10 years and 2643 (16.67%) with active lesions were observed to be of the 11-16 years age group. The diagnosis of the disease was done mainly on clinical and epidemiological criteria and by microscopic examination of amastigotes in scrapings and smears from ulcer region after fixing and staining with Giemsa stain. The author observed an epidemic of ZCL (Zoonotic cutaneous leishmaniasis) in 1997 at the Jhaljhao locality amongst the non-locals and non-immune workers of Bela-Awaran Road Project. Most of the children and adults of a Masjid-Madrissah of Jhaljhao were also found infected with wet lesions of CL. During the present study the ratio of incidence in male to female was found to be 72:28 because women mostly stay at home. Patients presented lesions on the skin ranging from single or multiple ulcers. The mean duration of lesion was 7 months to one year or more. Face was found to be more involved (41%) in the cases of CL, as compared with limbs (37%) and legs (22%). The highest incidence of the disease was during the winter and early spring. The clinical observations revealed that the lesions were of wet type in villages but of dry type at cities. The brief duration of lesions confirms the acute character of CL related to Leishmania tropica mostly in the cities which is usually described as dry, small and self-healing lesions mainly located at the face and occurring in old stable endemic foci of northern parts of the Province. However, wet lesions (caused by L. major) were observed in southern parts. It indicates that in the highly populated areas of the cities, man-to-man transmission is possible while in the less populated, scattered and far-flung areas, the role of animal reservoir is important.
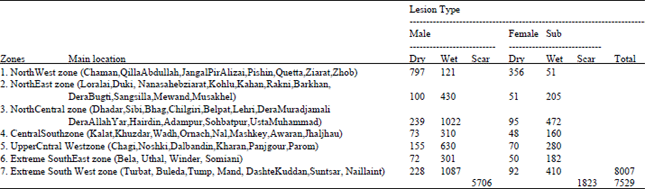
| Table 2: | Incidence of Cutaneous leishmaniasis in Balochistan Province, zoogeographic zone wise, according to sex and lesion type |
 | |
| Table 3: | Prevalence of Cutaneous leishmaniasis among school children (5-10, 11-16 years) in Balochistan Province |
 | |
| Table 4: | Results of Investigations on Rodents |
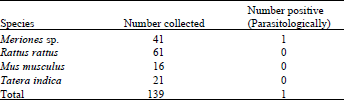 | |
Sandfly captures yielded 2013 sandflies. 23 species were taxonomically confirmed and 5 flies (&) were remained as undetermined species[41]. The flies identified in the endemic areas and near surroundings were Ph. papatasi, Ph. bergeroti, Ph. salehi, Ph. sergenti, Ph. alexandri, Ph. andrejevi, Ph. nuri, S. fallax, S. dentata arpaklensis, S. murghabiensis, S. mervynae, S. freetownensis Sinton var., S. babu babu, S. palestinensis, S. baghdadis, S. grekovi, S. clydei, S. tiberiadis pakistanica, S. punjabiensis, S. theodori pashtunica, S. hodgsoni hodgsoni, G. indica and G. dreyfussi turkestanica. Ph. papatasi (35.76%) was found to be more prevalent in all CL foci of the Province. However, in foci of northern and central parts of the Province, Ph. sergenti (7.95%) was also distributed. These both flies can be incriminated as the possible vector of CL in the region.
Live traps were placed at two hundred thirty two places and caught 139 rodents (Table 4). Rattus rattus (43.88%) appeared to be the predominant species in the region, Meriones with 30.2%, Tatera indica with 15.1% and Mus musculus with 11.5 % . None of these rodents trapped had shown any clinical evidence of disease. However, when smears were taken from rodent ears, one Meriones sp. showed to harbor amastigotes and the rest were found negative. Dedet et al. [42] and Rab et al.[28] have reported natural infection of CL in rodents without clinical symptoms.
In this study, the high frequency of severe lesions in children and elderly patients suggests that the introduction of the parasite occurred recently in new endemic foci and also in the old ones. The patients immune status associated with parasite factors probably play role in these peculiar clinical manifestations. However, one explanation to this is that no doubt refugees of Afghanistan as well as of Iran are not restricted to the campus but are rather scattered all over the Province and they too have a long history of CL. Factors determining the actual levels of endemicity include living conditions of these refugees and also of the rural people. They suffer a multitude of adversities just to survive and are constantly seeking better living condition, often ending up setting down in peri-urban settings and creating new foci of the disease, thus bringing the epidemic phenomenon to these urban areas. Also it is to be expected that increased incidence of the disease is also due to the destruction of the ecological habitat of the sandflies-vector and animal reservoir host (s) due to the urbanization of this part of the country.
It was noticed during the present survey that 40% of the CL patients stated that they used skin ointments but sore were not cured, 28% of the patients replied that they did not apply any medicine, 32% of the patients said that they applied extracts of local herbal and medicinal plants and the lesions were cured. Less than 1% of the patients explained that they applied Glucantime injection on the sore and the same was healed. In some cases ice piece were applied on the lesions and it was stated that it gave a good result. However, it was observed that patients who applied Glucantime injection, the scar of the CL became black pigmented and the patients who applied extracts of local herbal plants, the scar were of the same color as of their normal skin.
As far as the health Staff of the Government Hospitals and Private clinics are concerned, mostly were found unaware about even the biting habits of sandflies-vector, the transmitting agent of leishmaniasis and the name of the Glucantime injection, the only safe and reliable drug for the treatment of CL. Neither this drug was observed to be present in the Hospital nor it was found available in Medical Stores of the area except Quetta, Bela and Uthal localities.
It is concluded that it is necessary to start health education and awareness of the local population and a basic course about CL, its insect vectors and reservoir host (s) must be taught to the health staff working at local health institutions. Another necessity is parasite typing of this region as Rab[9] and Rab et al.[29] characterized the parasite from northern parts of the country as Leishmania infantum and L. tropica, respectively.
Reservoirs of the infections should be analyzed at locations where there is a high-risk group and a co-operation with the Malaria Eradication Program for eliminating the vector species should be established and started immediately. The extent and gravity of CL have to be expected and will remain a health problem unless effective control measures against sandflies and gerbils are put into effect. The control actions against CL are to be geared to breaking the chain of transmission between the infected rodents, the vector and man. Routine interventions, followed by epidemiological and entomological surveillance activities are necessary due to the presence of infected humans, Phlebotomus species and the presence of rodents in the areas where high densities of possible vector species is confirmed. Sufficient supply of the Glucantime injection especially to the Government Hospitals and Dispensaries must be maintained in the interest of the patients. Further, screening of extracts of medicinal plants in order to determine their anti leishmanial activity should also be started in the research laboratories of the Pakistani Universities as Glucantime injection is very costly and inaccessible to the patients living in far flung areas of the country.
The author is grateful to Professors Drs. R. Killick-Kendrick.; David, J. Bradley, R.W. Ashford, R.P. Lane and Dr. David Evans for their encouragement and valuable guidance on leishmaniasis and sandflies. My sincerest thanks are also due to respected Joanna Kapusta (BMNH), Linda Huddleston (BMNH), Dr. J.-P. Dedet (France) and Dr. Farrokh Modabber (WHO) and Prof. Dr. V. N. Neronov (Russia) for providing me the literature on leishmaniasis and sandflies.