ABSTRACT
Calcium channel blockers are increasingly used for the treatment of hypertension. Hypertension is an important risk factor for liver damage and several other circulatory abnormalities. The aim of this study was to determine the effects of lacidipine in a irradiation-induced hepatocellular damage model in Deoxyc Orticosterone Acetate (DOCA)-salt-induced hypertensive model in rats. In this study, animals were divided into five groups as follows: control (Group 1), hypertensive (Group 2), irradiated (Group 3), irradiated and hypertensive (Group 4) and irradiated, hypertensive and lacidipine-treated (Group 5). At the end of the experiment, the livers were removed and its homogenates were biochemically examined. Significant differences were found between values of all groups (p<0.05). Group 3 and particularly Group 4 showed significant increase in lipid peroxidation and Nitric Oxide (NO) and serum tumor necrosis factor-α (TNF-α) with a significant reduction in serum level of alanine amine transferase (ALT) enzyme and in superoxide dismutase in red blood cells lysates. Lacidipine-treated group (5) showed a significant reduction in elevated systolic blood pressure together with a great protection of ALT and SOD enzymes from the destructive effects of irradiation and hypertension. Additionally, this CCB reduces hepatic NO and serum TNF-α levels that were increased in groups (2,3,4). The present study suggests that lacidipine has some important protective effects on liver of hypertensive irradiated albino rats.
PDF Abstract XML References Citation
How to cite this article
DOI: 10.3923/pjbs.2013.1353.1357
URL: https://scialert.net/abstract/?doi=pjbs.2013.1353.1357
INTRODUCTION
The survival rates of cancer patients are extremely improved by radiotherapy (Bentzen, 2006). Meanwhile, those patients suffer from various hepatic disorders up to hepatocellular damage and an increase in risk of liver failure as well as many other important side effects (Bentzen, 2006). An increase in inflammatory cytokines as tumor necrosis factor-alfa (TNF-α). Interleukin-1, interleukin-6 is reported with irradiation-induced adverse effects as hepatocellular damage or bone loss (Park et al., 2004). Additionally, irradiation is always accompanied by an increase in serum cortisol level together with a reduction in antioxidant markers due to oxidative stress-induced by irradiation (Ozgocmen et al., 2007).
Calcium channel blockers (CCB) are commonly used in the treatment of many clinical disorders e.g. angina pectoris, myocardial infarction, arrhythmia, left ventricular diastolic dysfunction, Raynaud's syndrome, migraine, osteoporosis, esophageal spasm and subarachnoid bleeding (McIntyre et al., 1999; Yagmurdur et al., 2002; Galisteo et al., 2004; Halici et al., 2008).
Lacidipine is a L-type Calcium Channel Blocker (CCB). It is a very effective antihypertensive drug. In previous studies, it was proven to induce many beneficial effects in its different therapeutic uses that may be related to its antioxidant and Nitric Oxide (NO) modulation (Garzotti, 2003).
Hypertension is recognized as a "silent killer" disease whose pathogenesis includes the production of reactive oxygen species (ROS) by vascular cells and alterations in antioxidant enzymes (McIntyre et al., 1999). The antioxidant effects of CCBs against these harmful actions are not yet well recognized.
A study conducted in 1993 proved that dihydropyridine CCBs can modulate many inflammatory markers mediated via inhibition of induction of Nitric Oxide Synthase (NOS) enzyme. This inhibition prevents the production of detrimental NO by cultured macrophages under the effect of endotoxins (Szabo et al, 1993). This inhibitory effect protects against damage of the vascular endothelium especially in cases of atherosclerosis and hypertension with reduction in the risk of hypertension-related complications (Kunz, 2000; Chobanian et al., 2003).
Hypertension induces many vascular disorders in the liver which is a rich organ in blood supply. Irradiation has a hepatotoxic effect, however hepatic cells can regenerate themselves but this regeneration was found to be greatly reduced if the condition is accompanied by a vascular disease such as hypertension (Bentzen, 2006). Chronic radiation hepatitis is a serious adverse effect of exposure to irradiation (Mornex et al., 1997).
The literature about the effects of irradiation on the liver of hypertensive patients is still inadequate. The present study aimed to determine some possible hepatoprotective effects of lacidipine, as a dihydropyridine CCB, in irradiated albino rats.
MATERIALS AND METHODS
Materials: Lacidipine ester was provided as powder by GlaxoSmithKline, Philadelphia, PA, USA. Deoxycorticosterone acetate (DOCA) (Sigma chemicals co. available as powder suspended in corn oil). Superoxide dismutase enzyme [SOD] kit (RANSOD, by Randox Laboratories). ALT enzyme Kit was obtained from Biodiagnostic (Cairo, Egypt) and serum TNF-α ELISA was purchased from Ani Biotech. Finland. Any other chemical was purchased from Sigma Chemicals Co. Lisinopril was dissolved in 0.5% methylcellulose and it was freshly prepared.
Animal protocols: Sixty albino rats weighing 180-200 g, each were randomized into 5 groups [N = 12, in each group based on sample size done on microlab system using α<0.05 and β>80% values].
DOCA-Salt Hypertension (McIntyre et al., 1999). Thirty-six albino rats were treated twice weekly with DOCA and administered subcutaneously (15 mg kg-1) and 1% NaCl was added to their tap water for drinking. Two weeks after the start of DOCA-salt treatment, these rats were randomly divided into 3 groups (each group, n = 12).
Animal grouping:
| (Duration of the study = 8 weeks) |
| • | Group 1(Control non-treated): It received standard volume of 0.5% methylcellulose equal to that injected in lacidipine-treated rats as a solvent of lacidipine |
| • | Group 2:It was DOCA-induced hypertensive rats without any treatment. [Rats are already rendered hypertensive as mentioned above] |
| • | Group 3 (Irradiated group): It was exposed to 15 Gy whole body γ-irradiation fractionated over 8 weeks (3Gy/week, 1Gy day after day) using the facilities of Misr Center for Radiation-Egypt using Cesium-137 irradiation unit (Gamma cell-40) produced by the Atomic Energy of Cananda Limited at a dose rate of 0.46 Gy min-1 |
| • | Group 4: It was DOCA salt- induced hypertension+γ-irradiation as mentioned above in groups 2 and 3 |
| • | Group 5:It was DOCA salt- induced hypertension+γ-irradiation as mentioned above in groups 2 and 3 + Lacidipine in a dose of 1 mg kg-1 day-1 ip for 8 weeks |
Assessment of Systolic Blood Pressure (SBP) changes (Bunag, 1973): SBP was measured by a tail-cuff sphygmomanometer (UR-5000, Ueda Co, Ltd, Japan). SBP measurements were conducted before starting treatment with lisinopril then at the end of the 8th week of treatment. Measurements were made at 2:00 to 5:00 p.m. (5 to 6 h after treatment administration) to minimize circadian influences. For each animal an average of at least three consecutive measurements was taken to reduce variability.
At the end of the 8th week, each rat was anesthetized with urethane [1 mg kg-1 i.p.], slaughtered and liver was removed and divided into 2 parts, part of it was homogenized for TBARS measurement and the other part was used to measure liver tissue content of NO as total nitrite (NOx). Additionally, blood samples were collected from rats of all groups for measurement of serum ALT enzyme and TNF-α levels, SOD enzyme concentrations in erythrocyte lysates using commercially available colorimetric assay kit.
Measurement of serum levels of alanine amine transferase (ALT) enzyme: Serum levels of ALT was measured using biochemistry automatic analyzer (Hitachi7600).
Measurement of hepatic thiobarbituric acid-reactive substances (TBARS) as a marker of lipid peroxidation (Gutteridge and Quinlan, 1983): Liver homogenates were rinsed with cold 0.14 M sodium chloride and homogenized in 25% ice-cold 50 mM Tris-HCl buffer (pH 7.4). A 150 μL of the tissue supernatant of samples were diluted to 500 μL with deionized water. Two-hundred and fifty microlitter of 1.34% thiobarbituric acid was added to each tube, followed by the addition of an equal volume of 40% trichloroacetic acid. The mixtures were then shaken and incubated for 30 min in a boiling water bath. Tubes were allowed to cool to room temperature and the absorbance was then read at 532 nm, using zero concentration.
Measurement of liver tissue of NO ( Green et al., 1982): Liver tissue content of NO was measured as total nitrite (NOx), the stable degradation products of NO, after reduction of nitrate to nitrite by copper-cadmium alloy and measuring total nitrite (nitrite+nitrate) using Griess reagent.
Determination of SOD enzyme level in erythrocyte lysates: At the end of the study, blood samples were collected from rats from all groups for measurement of SOD levels in erythrocyte lysates, using commercially-available colorimetric assay kits, based on an indirect xanthine-xanthine oxidase (Halliwell and Chirico, 1993) and results were expressed in IU mL-1.
Measurement of serum TNF-α as a pro-inflammatory mediator: Serum TNF-α was assayed using ELISA reagent kit.
Protein determination: The protein content of liver homogenates was determined by spectrophotometer according to the method of Bradford (1976). The aim is to relate the oxidative marker concentrations to the total tissue protein.
Data analysis: The results are presented as mean± Standard Deviation (SD) and evaluated using one-way analysis of variance (ANOVA), followed by Tukey’s post hoc determination, using GraphPad Prism (version 3.00; GraphPad Software, La Jolla, CA, USA).
RESULTS
| • | Effect of lacidipine on Systolic Blood Pressure (SBP) in irradiated DOCA-salt treated albino rats SBP was significantly (p< 0.05) lowered by lacidipine (group 5) compared to non-treated irradiated DOCA-salt administered albino rats (group 3 and 4). Results were comparable to that reported with control rats (group 1) (Fig. 1). The mean±SD of SBP for each group remained constant all over the 8-hours period of measurement of SBP |
| • | Effect of lacidipine on serum ALT in U L-1 and liver tissue contents of TBARS in nmol mg-1 tissue protein and liver tissue NOx in μM g-1 and SOD in IU mL-1 RCs lysates in irradiating DOCA-salt treated hypertensive albino rats (Table 1) |
| • | Effect of lacidipine on serum serum TNF-a in Pg mL-1 of irradiated DOCA-salt treated hypertensive albino rats (Table 2) |
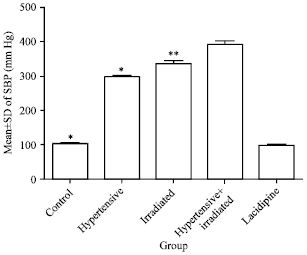 | |
| Fig. 1: | Effect of lacidipine on Systolic Blood Pressure (SBP) on irradiated DOCA-salt treated albino rats, *Significant (p<0.05) increase in SBP in DOCA-salt treated without lacidipine (group 2-4) compared to group 1, **Significant (p<0.05) decrease in SBP in lacidipine-treated group (5) compared to group 2-4 |
| Table 1: | Showed a significant (p<0.05) reduction in TBARS and in serum ALT concentration with a decrease in liver NOx, SOD enzyme level in RBC lysates in lacidipine-treated group (5) in comparison to the untreated hypertensive and/or irradiated group (2,3,4) |
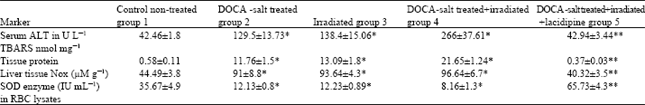 | |
| *p<0.05 significant increase in TBARS and serum ALT concentration and liver NOx with reduction in SOD enzyme level in groups (2, 3, 4) compared to the control non-treated group (1) **p<0.05 significant reduction in TBARS with decrease in ALT enzyme concentration and liver NOx and SOD enzyme level in RBCs lysates of lacidipine-treated group (5) in comparison to groups (2,3,4) | |
| Table 2: | Showed a significant (p<0.05) reduction in serum TNF-α concentration in lacidipine-treated group (5) in comparison to the untreated hypertensive and/or irradiated group (2,3,4) |
| *p<0.05 significant increase in serum TNF-α concentration in groups (2,3,4) compared to the control non-treated group (1) , **p<0.05 significant reduction in TNF-α concentration of lacidipine-treated group (5) in comparison to groups (2, 3, 4) | |
DISCUSSION
Exposure of DOCA-salt treated hypertensive albino rats to γ-irradiation, in the present study, revealed a significant increase in hepatic TBARS , a marker of lipid peroxidation, an elevation in deleterious NOx content and in serum level of TNF-α with a significant reduction in serum levels of ALT enzyme and SOD enzyme in RBCs lysates. Eight-weeks treatment with lacidipine, as once daily dose, reverses all the above mentioned results with improvement of the detrimental effects induced by γ-irradiation on albino rats.
The radiation-induced liver disease, often called radiation hepatitis, occurs approximately 2 weeks to 4 months after hepatic irradiation. The late lesions may be associated with signs of chronic radiation hepatitis (Mornex et al., 1997). Radiation-induced hepatic injury is a form of veno-occlusive disease due to fibrous obliteration of the terminal hepatic venules leading to postsinusoidal obstruction (Lawrence et al., 1995).
In an attempt to explain the results of the present study , Similar experimental studies demonstrated a state of chronic oxidative stress in lungs of rats exposed to γ-irradiation (Vujaskovic et al., 2001). Hypoxia was induced in the rat lung by the administration of a single dose of 28 Gy for 6 weeks. There were significant increase in macrophage activity, fibrosis and production of pro-inflammatory mediators in the post-irradiation period. Hypoxia has been shown to lead to Increased Reactive Oxygen Species (ROS) production with a significant reduction in antioxidant and/or antioxidant enzyme production e.g., Super Oxide Dismutase enzyme (SOD) (Li and Jackson, 2002).
An increase in malondialdehyde levels, as a marker of lipid peroxidation, was reported in the lungs of mice after exposure to γ-irradiation. These mice were described to be exposed to a model of radiation-induced chronic oxidative stress (Kang et al., 2003).
Lacidipine, as a one of dihydropyridine Calcium Channel Blockers (CCBs), is an effective antihypertensive drug together with its great efficacy in reducing vascular Intima-Media Thickness (IMT) than other classes of antihypertensive drugs due to their vascular effects. An experimental study in 2012 revealed that 30 μM lacidipine inhibited about two-thirds of the oxidized-low density lipoprotein (ox-LDL). This ox-LDL has a major role in induction of ROS production. This study has demonstrated that lipophilic CCB, lacidipine, may inhibit ox-LDL induced proliferation and oxidative stress of vascular smooth muscle cells (VSMCs) (Zou et al., 2012). This anti-oxidant effect could be implicated on the results of the present study as the increase in SOD enzyme content in association with a significant reduction in hepatic lipid peroxidation.
Another study evaluated the extent to which lacidipine possessed antioxidant properties. The authors investigated the expression of intercellular cell adhesion molecule-1 (ICAM-1), vascular cell adhesion molecule-1 (VCAM-1) and E-selectin on human umbilical vein endothelial cells, induced by different pro-oxidant signals such as oxidized Low Density Lipoprotein (LDL) and tumor necrosis factor-alpha (TNF-alpha) in the presence of this lipophilic CCB.
Results of this study showed that the incubation of 5 μ mol L-1 Cu2+-oxidized LDL not only caused a dose-dependent increase in ICAM-1, VCAM-1 and E-selectin), but also synergically increased their TNF-alpha-induced expression. The addition of lacidipine to human umbilical vein endothelial cells significantly reduced the expression of ICAM-1, VCAM-1 and E-selectin induced by TNF-alpha alone or with oxidized LDL These results pointed to the inhibitory effect of lacidipine to the pro-inflammatory mediators such as TNF-α and nitric oxide. So, lacidipine may have protective and therapeutic effects in atherosclerosis as a disease associated with pro-inflammatory mediators and oxidative stress.
Similarly, the present study could conclude that lacidipine could provide a hepatoprotective effect against pro-inflammatory mediators and lipid peroxidation induced by exposure of albino rats to 8-weeks γ-irradiation as it possessed an inhibitory effect to ROS as well as to the pro-inflammatory mediators in addition to its powerful vascular protective effect as an effective antihypertensive drug.
ACKNOWLEDGMENT
This research was supported by the Medical Research Service of the Ain Shams University, Cairo, Egypt. It was supported by the Laboratory of the Pharmacology Department, Faculty of Medicine, Ain Shams University, Cairo, Egypt. The author is grateful to staff of Misr Center for Radiation, Cairo, Egypt for their kind efforts done in the irradiation process of albino rats.
REFERENCES
- Bentzen, S., 2006. Preventing or reducing late side effects of irradiation therapy: Radiobiology meets molecular pathology. Nat. Rev. Cancer, 6: 702-713.
CrossRefDirect Link - Park, Y.G., S.K. Kang, W.J. Kim, Y.C. Lee and C.H. Kim, 2004. Effects of TGF-beta, TNF-alpha, IL-beta and IL-6 alone or in combination and tyrosine kinase inhibitor on cyclooxygenase expression, prostaglandin E2 production and bone resorption in mouse calvarial bone cells. Int. J. Biochem. Cell Biol., 36: 2270-2280.
PubMed - Ozgocmen, S., H. Kaya, E. Fadillioglu, R. Aydogan and Z. Yilmaz, 2007. Role of antioxidant systems, lipid peroxidation and nitric oxide in postmenopausal osteoporosis. Mol. Cel. Biochem., 295: 45-52.
CrossRefDirect Link - McIntyre, M., D.F. Bohr and A.F. Dominiczak, 1999. Endothelial function in hypertension: The role of superoxide anion. Hypertension, 34: 539-545.
Direct Link - Yagmurdur, M.C., A. Ozdemir, S. Topaloglu, K. Kilinc and A. Ozenc, 2002. Effects of alpha tocopherol and verapamil on liver and small bowel following mesenteric ischemia-reperfusion. Turk J. Gastroenterol., 13: 40-46.
PubMedDirect Link - Galisteo, M., M.F. Garca-Saura, R. Jimenez, I.C. Villar, A. Zarzuelo, F. Vargas and J. Duarte, 2004. Effects of chronic quercetin treatment on antioxidant defence system and oxidative status of deoxycorticosterone acetate-salt-hypertensive rats. Mol. Cell. Biochem., 2: 91-99.
PubMedDirect Link - Halici, Z., B. Borekci, Y. Ozdemir, E. Cadirci and H. Suleyman, 2008. Protective effects of amlodipine and lacidipine on ovariectomy-induced bone loss in rats. Eur. J. Pharmacol., 579: 241-245.
CrossRefDirect Link - Garzotti, M., 2003. Lacidipine, a potential peroxynitrite scavenger: Investigation of activity by liquid chromatography and mass spectrometry. Rapid Commun. Mass Spectrom., 17: 272-278.
CrossRefDirect Link - Szabo, C., C. Thiemermann and J.R. Vane, 1993. Dihydropyridine antagonists and agonists of calcium channels inhibit the induction of nitric oxide synthase by endotoxin in cultured macrophages. Biochem. Biophys. Res. Commun., 196: 825-830.
CrossRefDirect Link - Kunz, J., 2000. Initial lesions of vascular aging disease (arteriosclerosis). Gerontology, 46: 295-299.
CrossRefDirect Link - Chobanian, A.V., G.L. Bakris, H.R. Black, W.C. Cushman and L.A. Green et al., 2003. The seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure: The JNC 7 report. J. Am. Med. Assoc., 289: 2560-2571.
CrossRefPubMedDirect Link - Mornex, F., F. Gerard, O. Ramuz and P. Van Houtte, 1997. Late effects of radiations on the liver. Cancer Radiother., 1: 753-759.
CrossRefPubMedDirect Link - Green, L.C., D.A. Wagner, J. Glogowski, P.L. Skipper, J.S. Wishnok and S.R. Tannenbaum, 1982. Analysis of nitrate, nitrite and [15N] nitrate in biological fluids. Anal. Biochem., 126: 131-138.
CrossRefPubMedDirect Link - Halliwell, B. and S. Chirico, 1993. Lipid peroxidation: Its mechanism, measurement and significance. Am. J. Clin. Nutr., 57: 715S-724S.
Direct Link - Bradford, M.M., 1976. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal. Biochem., 72: 248-254.
CrossRefPubMedDirect Link - Lawrence, T.S., J.M. Robertson, M.S. Anscher, R.L. Jirtle, W.D. Ensminger and L.F. Fajardo, 1995. Hepatic toxicity resulting from cancer treatment. Int. J. Radiat. Oncol. Biol. Phys., 31: 1237-1248.
PubMedDirect Link - Vujaskovic, Z., M.S. Anscher, Q.F. Feng, Z.N. Rabbani and K. Amin et al., 2001. Radiation-induced hypoxia may perpetuate late normal tissue injury. Int. J. Radiat. Oncol. Biol. Phys., 50: 851-855.
PubMedDirect Link - Li, C. and R.M. Jackson, 2002. Reactive species mechanisms of cellular hypoxia-reoxygenation injury. Am. J. Physiol. Cell Physiol., 282: C227-C241.
CrossRefPubMedDirect Link - Kang, S.K., Z.N. Rabbani, R.J. Folz, M.L. Golson and H. Huang et al., 2003. Overexpression of extracellular superoxide dismutase protects mice from radiation-induced lung injury. Int. J. Radiat. Oncol. Biol. Phys., 57: 1056-1066.
CrossRefPubMedDirect Link - Zou, J., Y. Li, H.Q. Fan and J.G. Wang, 2012. Effects of dihydropyridine calcium channel blockers on oxidized low-density lipoprotein induced proliferation and oxidative stress of vascular smooth muscle cells. BMC Res. Notes.
CrossRefDirect Link








