Research Article
The Effect of Caesarian Section in Preventing Postpartum Stress Urinary Incontinence in Primiparous Women after One Year of Delivery
Department of Ob-Gyn, Lorestan University of Medical Sciences, Lorestan, Iran
Women are confronted with certain situations that affect their life, the most important of which is probably pregnancy followed by delivery and the postpartum period.
Pregnancy causes functional and structural changes in the female urogenital organs (Bump and Norton, 1998; Marshall et al., 1998).
Most of these changes render women prone to disease or exacerbate the previously existing conditions (Tomezsko and Sand, 1997; Chaliha and Stanton, 2002). One of these problems is urinary incontinence that not only affects the quality of life, but also causes considerable expenses for treatment urinary incontinence is a disabling condition manifesting as involuntary discharge of urine, leading to hygiene and social problems. Pregnancy and delivery are major causes in favors of incontinence (Thorp et al., 1999). Most women experience their first episode of urinary incontinence during pregnancy. Vaginal delivery may also be another risk factor for urinary incontinence (Nygard, 2006).
Urinary incontinence is a common problem in pregnancy, affecting 30-60% of women, as a result of uterine enlargement, hormonal changes, glumeral filtration rate rise, transient changes in the urethral angle and other physiologic conditions. Urinary incontinence associated with pregnancy usually resolves spontaneously, but it may persist in some cases (Burgio et al., 2007).
According to Burgio et al. (2003), urinary incontinence after delivery is significantly associated with pathophysiological changes of delivery such as bladder trauma, neuromuscular lesions and injury of the urethral sphincter.
The most common forms of urinary incontinence are urge incontinence, stress incontinence and mixed incontinence. The risk factors for the stress type are not fully known, but factors such as delivery, weight, age, ethnicity, pelvic surgeries, smoking history and conditions raising the intra abdominal pressure have been incriminated. Earlier studies suggest that urinary incontinence following delivery is a multifactorial condition, associated with previous urinary incontinence, pregnancy urinary incontinence, high body mass index before pregnancy, vaginal delivery, using forceps and number of parity (Eason et al., 2004; Hvidman et al., 2003; Pregazzi et al., 2002).
Stress urinary incontinence in young women usually follows pelvic floor injury during the process of normal delivery. The role of caesarian in preventing such injuries is controversial. We conducted a prospective study to compare the prevalence of Stress Urinary Incontinence (SUI) in primiparous women undergoing spontaneous vaginal delivery with elective caesarian or caesarian after obstructed labor, for one year after the first delivery.
In a cohort, prospective study, 330 primiparous women referring to Asali Charity Hospital for spontaneous vaginal delivery, elective caesarian or caesarian after obstructed labor (emergency) during February and March 2006 were categorized in three groups. The exclusion criteria are as follows:
| • | Women with urinary incontinence before pregnancy |
| • | Women with background conditions such as renal disease, hypertension, diabetes before or during pregnancy |
Thus, only the cases of stress urinary incontinence due to delivery were included. The patients were categorized in three groups based on their type of delivery:
| • | Spontaneous vaginal delivery (120 cases) |
| • | Elective caesarian (110 cases) |
| • | Caesarian after obstructed labor (100 cases) |
The average cervical dilation and duration of obstruction for caesarian after obstructed labor were 8.7±1.6 cm and 184±24 min, respectively.
Prevalence, frequency and intensity of stress urinary incontinence were analyzed in the three groups, as well as obstetric and demographic parameters. The patients were studied for intensity of incontinence immediately after delivery and 1 month, 3 months, 6 months and 1 year later. The sampling tool was a questionnaire and the data were analyzed using Chi-squared, one-way ANOVA and logistic regression tests and p<0.05 was considered significant.
The primary evaluations of maternal age and weight using the one-way ANOVA and two-by-two comparison test revealed that the cases are different in terms of weight and age. Therefore, the weight and age factors were used as confounding factors in the regression-logistic test. Also the elective caesarian was used as the basis for comparison.
The Chi-squared independence test indicates that there is a significant relationship between the incidence of stress urinary incontinence and the type of delivery (p = 0.460), with a confidence of 93.6%.
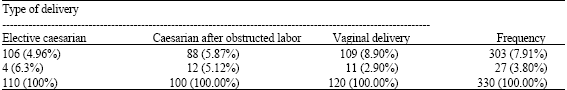
| Table 1: | Distribution of frequency of patients based on the type of delivery and the incidence of SUI after delivery |
 | |
| Table 2: | Results of the regression-logistic test based on the odds ratio (OR) |
 | |
Also the trend test reveals that the incidence of stress urinary incontinence rises in the order of elective caesarian, caesarian after obstructed labor and vaginal delivery p = 0.50) (Table 1).
These result depict that generally the age and weight of women is not effective in the incidence of stress urinary incontinence after delivery (p = 0.531 and p = 0.988) (Table 2). However, there is a confidence of 90% that the type of delivery is effective in the incidence of stress urinary incontinence (p = 0.108) with the chance of developing SUI following caesarian after obstructed labor 3.6 times larger than that of elective caesarian (CI = 1.1-11.8) (p = 0.035) while the chance of developing SUI after vaginal delivery is 2.6 times larger than that of elective caesarian (p = 0.105), which may be significant with 10.5% error (insignificant at the level of α = 0.05).
The chances of developing SUI following vaginal delivery and caesarian after obstructed labor are nor significantly different (p = 0.502).
In this study, the frequency of urinary incontinence one year after spontaneous vaginal delivery was 9.2%, a figure reported to be 11.6% in Burgio et al. (2003) at 6 weeks and not changing significantly after 1 year. Another study in the Netherlands reported such frequency to be 26% at 38 weeks of gestation, 16% at 6 weeks of delivery and 15% at 6 months of delivery. Wijma et al. (2003) reported 22% stress urinary incontinence after 1 year of delivery, more frequent than this study reveals. The most powerful predicting factor is urinary incontinence 4-8 weeks after delivery (Schytt et al., 2004). In this study, the frequency of urinary incontinence was not significantly associated with maternal age and weight. An Italian study reported high maternal weight at the onset of pregnancy as a significant risk factor (Pregazzi et al., 2002), while another study did not indicate such a relationship, similar to this study (Peyrat et al., 2002).
Pregazzi et al. (2002) reported the prevalence of urinary incontinence to be 8.2% in primiparous and 20% in multiparous women, indicating a significant relationship between the number of parity and prevalence of urinary incontinence. An increasing number of parity leads to weakening of pelvic muscles and a higher prevalence of urinary incontinence, corroborated in various studies. Therefore, we performed this study only in primiparous women to eliminate this confounding factor.
This study reveals a significant relationship between stress urinary incontinence in vaginal delivery and caesarian. The prevalence of SUI is almost identical in spontaneous vaginal delivery and caesarian after obstructed labor; it is probable that the extensive pelvic floor injury in the latter is irreparable with surgical intervention-caesarian section (Marshall et al., 2002).
On the other hand, elective caesarian without undergoing labor was significantly associated with a lower frequency of SUI. In the study, performed by Groutz et al. (2004) the frequency of stress urinary incontinence was similar in spontaneous vaginal delivery and caesarian after obstructed labor, while it was significantly lower with elective caesarian, similar to our findings (Rortveit et al., 2003) reported the risk of urinary incontinence is higher among women who have had cesarean sections than among nulliparous women and is even higher among women who have had vaginal deliveries. However, these findings should not be used to justify an increase in the use of cesarean sections.
According to numerous studies, including ours, vaginal delivery is a risk factor for SUI. However, the role of pregnancy is yet to be defined. The impact of delivery has been described in the following ways (Hvidman et al., 2003):
| • | The first delivery in the form of caesarian section has a preventive role, although subsequent caesarian tend to decrease this effect |
| • | The first vaginal delivery especially using forceps has a deteriorating effect and raises the risk of SUI, although subsequent vaginal deliveries do not raise the risk considerably |
| • | A difficult delivery necessitating emergent caesarian causes injuries to the nerves and muscles of the pelvic floor, especially to the pudendal nerve in the alcock canal near the ischial spine, disrupting the function of muscles such as levator ani, leading to the consequent disruption of urogenital and anal sphincters (Burgio et al., 2007) |
The findings of this study indicate that the frequency of SUI is similar with spontaneous vaginal delivery and caesarian after obstructed labor, while elective caesarian is significantly associated with a lower risk of stress urinary incontinence. Whether or not elective caesarian is indicated to prevent pelvic floor injury is still open to debate.